Creativity requires the courage to let go of certainties. Erich Fromm

Creativity requires the courage to let go of certainties. Erich Fromm


Dancing is the poetry of the foot. John Dryden
Interesting article from ScienceAlert.
Link to article: https://www.sciencealert.com/giving-up-your-phone-for-just-3-days-can-reshape-your-brain-activity
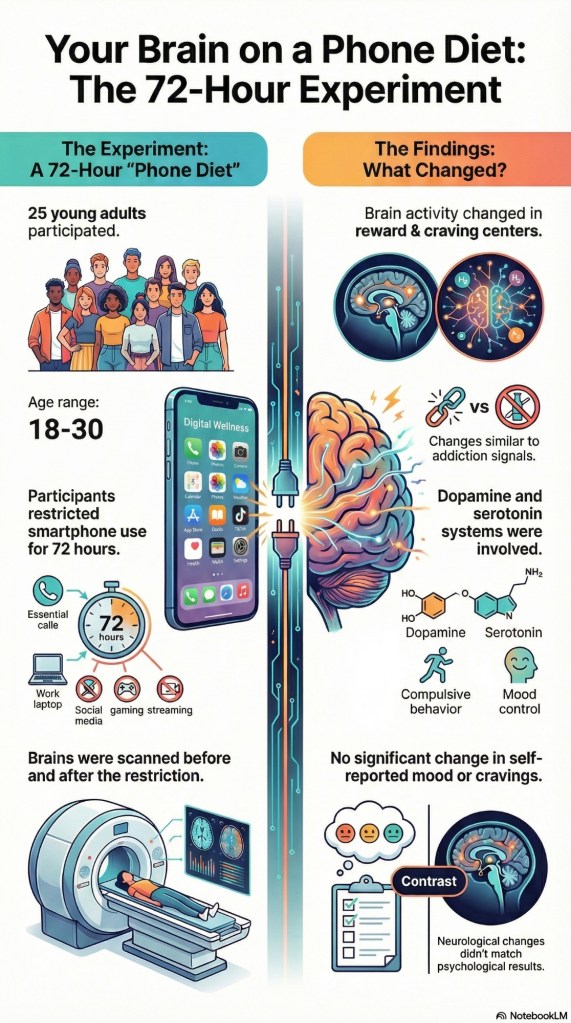
Researchers from German universities investigated 25 young adults who limited their phone use to essential tasks for 72 hours, using MRI scans and psychological tests before and after the restriction period. The core finding was that images of smartphones after the restriction triggered changes in brain regions associated with reward processing and cravings, similar to patterns observed in substance addictions. These neural changes were specifically linked to dopamine and serotonin systems, supporting the hypothesis that excessive smartphone use can be addictive. Although brain activity showed these changes, the psychological tests did not register significant changes in the participants’ mood or reported cravings during the brief period of restriction.